Figure 1 Quiz of the Week
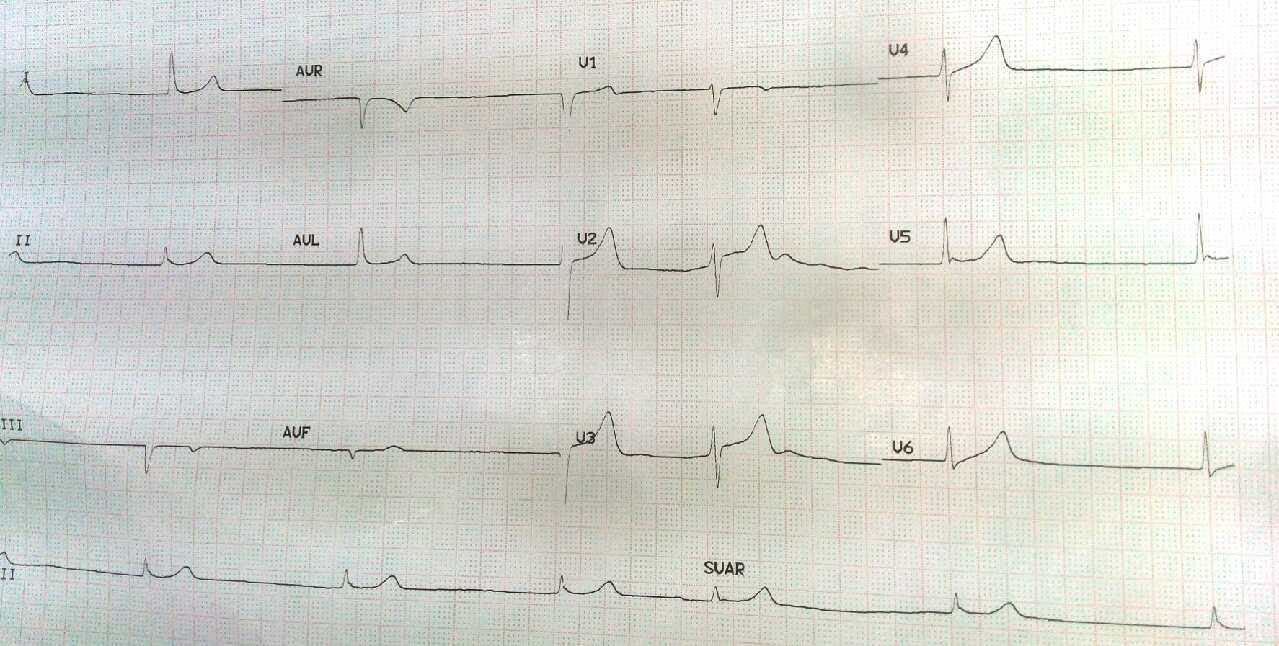
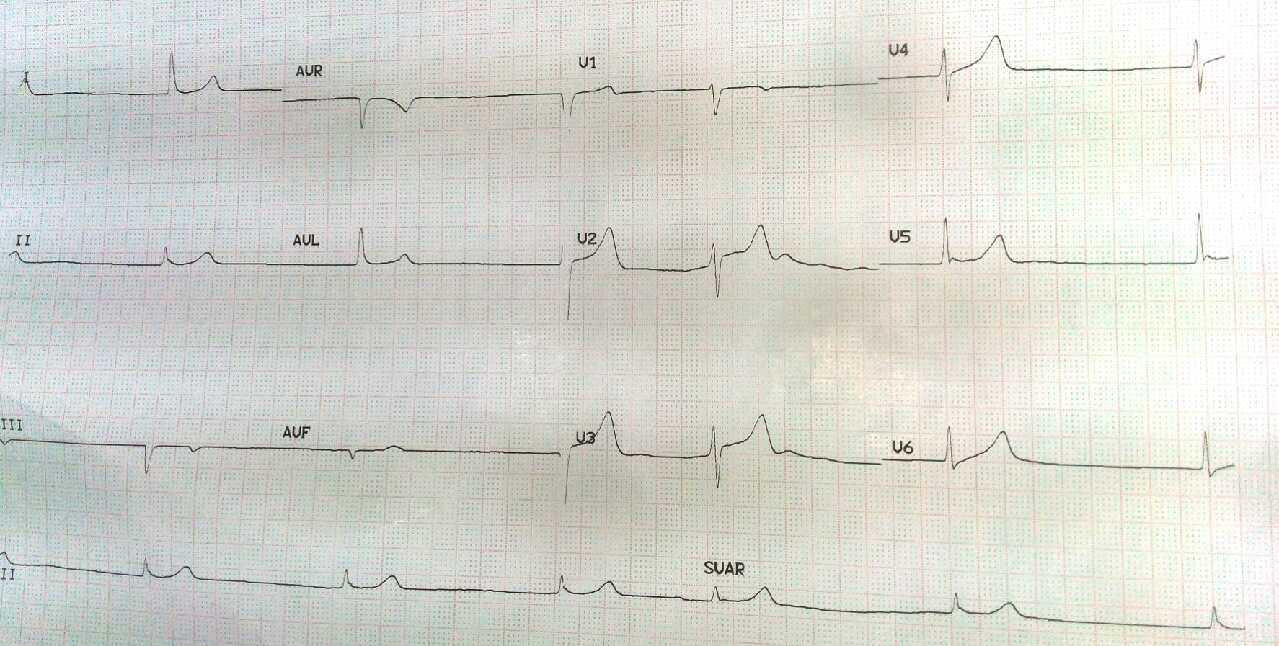
A 70-year-old male is brought to the emergency department with subacute shortness of breath and fatigue. Upon searching her father’s home, his daughter reports she found his medication — a nearly empty bottle of metoprolol, 100 mg bid. She believes her father has coronary artery disease. On examination, the patient is confused. His blood pressure is 69/49 mmHg and he has a heart rate of 48 bpm. An ECG reveals the findings seen here.
Image credit: @ParantapJTrivedi.
Answer: Glucagon
This patient’s presentation is suggestive of subacute beta blocker toxicity. Patients with chronic or acute overuse most often present with hypotension and bradycardia. After initial management, glucagon is the recommend first-line therapy for patients with beta blocker toxicity. Additional medications like calcium salts, catecholamines, and high-dose insulin (with glucose) may be given if the patient is severely symptomatic or refractory to glucagon. The most important step occurs after resuscitation — removing the offending agent and reestablishing a safe dose.
Read more and join the discussion now at Figure 1!
Explore cases, quiz yourself, and solve medical mysteries along with thousands of other medical professionals around the world on Figure 1, the free app where doctors expand their clinical knowledge.